Hip Dysplasia in dogs is a common yet complex disease. Although associated with large breed dogs, it also occurs in small dogs. As responsible pet parents, we should learn everything we can about this disease and how to avoid it.
Early diagnosis is vital and starts by identifying your dog’s risk, as well as learning to spot early symptoms.

Keep scrolling to find out why this illness happens to our dogs and how to prevent it from becoming severe.
Quick Navigation
- 1 What is Hip Dysplasia in dogs?
- 2 What causes Hip Dysplasia in dogs?
- 3 Signs of Hip Dysplasia in dogs
- 4 How is Hip Dysplasia in dogs diagnosed?
- 5 Treatment for Hip Dysplasia in dogs
- 6 How can you reduce the risk of Hip Dysplasia?
- 7 Life for dogs with Hip Dysplasia
- 8 The verdict about Hip Dysplasia in dogs
- 9 Further reading: Other diseases and conditions in dogs
- 10 Reference
What is Hip Dysplasia in dogs?
This skeletal deformity, also known as Canine Hip Dysplasia (CHD), develops as young dogs grow.
It’s often confused with arthritis, which has similar symptoms. But arthritis is due to old age.
Dysplastic dogs can develop arthritic changes in their joints as they physically mature. CHD interferes with the formation of hip sockets which can cause orthopedic mobility issues and Hip Dysplasia.
What causes Hip Dysplasia in dogs?
This developmental disease has two causes: genetics and diet. It progresses through various stages and affects the ball-and-socket joints of your dog’s hip, causing them to grow at equal rates.
The acetabulum (or hip joint) and head of the femur don’t function to enable easy movement. Instead, continued grinding causes joint degeneration. If left untreated, this leads to a loss of normal hip function.
Improper development first causes instability, or “looseness” of the joint, called joint laxity, that can progress to Degenerative Joint Disease (DJD) or Osteoarthritis.
DJD happens when dogs wear out their hip cartilage. It can be because it’s compensating for increasing laxity. Small fractures occur, forming scar tissue.
As the disease progresses, joint ligaments weaken, the bones grow too far apart, and become misaligned.
Deposits of calcium grow in these abnormal gaps causing bone spurs and hip pain.

When do dogs develop Hip Dysplasia?
CHD doesn’t choose gender, but giant breeds have a natural vulnerability to developing joint problems because of their weight.
It doesn’t choose between purebred and mixed-breed puppies, too. Some get Hip Dysplasia as early as 3 months of age, while others notice any problems until after a few years.
Is Canine Hip Dysplasia genetic?
This may be the most common orthopedic disorder in medium- to large-sized breeds, but their pedigree contributes, as well.
Those with a history of unregulated breeding are more at risk – more than 70% of purebred dogs are affected.
In most dogs, CHD is hereditary. Genetics is responsible for producing hormones that control the growth and development of all internal systems.
Genes that cause excessive growth can put a dog at risk of developing Hip Dysplasia, even if they haven’t inherited the actual condition.
Pure-breed dogs are more likely to be inbred, and dogs heavier than 50 lbs (22.5 kg) are also at risk.
The disease affects the following pedigree breeds in no particular order:
- German Shepherds
- Rottweilers
- Labrador Retrievers
- Golden Retrievers
- Saint Bernards
- Old English Sheepdogs
- Newfoundlands
- Mastiffs
- Bulldogs
- Pugs
- Otterhounds
- Basset Hounds
- Bloodhounds
- Chows
- Great Danes
Mixed-breeds are also susceptible to getting CHD, especially if their parents are any of the above breeds. The most vulnerable breed combinations are:
- Boxer-Lab mix (AKA Boxador)
- German Shepherd-Rottweiler mix (AKA Shottie)
- Retriever breeds

Can environmental factors cause CHD?
Your dog’s first year of diet and exercise has a long-term effect on their health. With that said, nutritional and physical factors can cause Hip Dysplasia.
People sometimes overfeed large puppies to make them bulky. Some people think it’s cute, but high-calorie diets and rapid weight gains, and eventually, obesity.
It can interfere with the dog’s growing bones and cause joint problems later on.
Lack of proper nutrients also puts them at risk of improper bone, joint, and muscle development. So it’s essential to strike a balance between high-quality nutrition and caloric intake.
Don’t forget the amount and type of exercise during your puppy’s first year or before its bones are fully developed.
If your fido is a couch potato, it prevents the muscles and ligaments from getting stronger. Too much exercise can also cause damage to the joints.
It’s best to limit your doggo from jumping on high and hard surfaces within the age of 12 to 18 months.
Wait until your dog is full-grown before doing intense and prolonged physical activities like taking them to run while you jog or cycle.

Signs of Hip Dysplasia in dogs
Irregular hip looseness at 2 weeks of age is the most common sign of Hip Dysplasia in puppies. But there are cases where dogs with tight hips developed CHD.
Oncoming lameness may make dogs weaker and less tolerant to exercise, but some dogs get the disease without showing any sign of lameness.
As a degenerative condition, it can take years for dogs to develop noticeable Hip Dysplasia symptoms. These can differ depending on your dog’s growth development stage.
These phases are Juvenile, at less than 18 months, and mature after that.
Here are more symptoms of Hip Dysplasia in dogs that can develop from youth to old age.
- Stiffness
- Pain
- Reduced activity
- Limited range of motion
- Swaying
- Limping
- Weight compensation & increased muscle around the favored limb
Bug is a gorgeous pup with CHD and a resulting irregular gate. Watch this video to see how the condition affects her range of motion.
In juvenile dogs, bunny-hopping is a sign of gait impairment. It’s where both hind legs are lifted while walking, running, or climbing stairs. It seems innocent enough, but it could be a sign of discomfort or pain.
This can also be the issue if a pup’s shifting its weight to its front legs or showing signs of lameness in one or both of its back legs.
Other indications of juvenile CHD include difficulty standing and an audible clicking sound originating in their hips when they do so.
Take note of any history of lameness and joint dislocation in your dog’s rear limbs. This increases the likelihood of developing mature Canine Hip Dysplasia.
You may observe them showing signs of reluctance when faced with physical activity, such as jumping, standing, and climbing stairs.
Stiff muscles in the morning and lameness after an activity can be a sign of hip problems in older dogs. They’re also susceptible to loss of muscle mass in their hind legs when affected by this disorder.
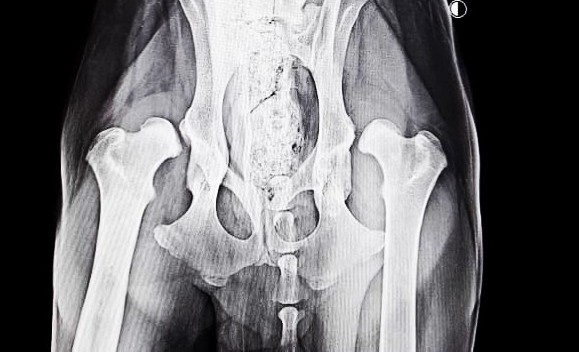
How is Hip Dysplasia in dogs diagnosed?
Diagnosing CHD early usually depends on owners noticing changes in their pet’s behavior. If so, take the dog to the veterinarian as soon as possible for a physical examination.
The vet will check for indications of looseness in the hips, reduced range of motion, blood tests, and electrolyte analysis. Urinalysis is also done to help detect possible inflammation.
Providing your dog’s medical history records is vital for diagnosis, including the information of his parents and previous injuries.
An X-ray or Radiographs will allow vets to see how severe your dog’s condition is, and it will help them decide the best course of treatment.
Tests for Canine Hip Dysplasia
There are two American protocols used to test for Canine Hip Dysplasia. These are the Orthopedic Foundation for Animals (OFA) protocol and the PennHip method.
Both assess the chances of a dog developing orthopedic problems such as CHD.
The OFA method is the most used US procedure for dogs who are at least 2 years old. In severe cases, this may be too late to prevent the worst of this condition from already developing.
The quantitative PenHip is more accurate. Remember, these are predictive tests that don’t take into account possible environmental factors.
There are pros and cons to both methods. Always consult with your veterinarian about your dog’s circumstances.
| Orthopedic Foundation for Animals (OFA) protocol | PennHIP protocol | |
| Age of screening | At least two years old | As young as four months old |
| Need for sedation | Unnecessary for most | Required for all dogs |
| Certification requirements | All veterinarians can perform it | Special certification needed |
| Predictive validity | Not guaranteed | Found to be more accurate |
| Costs | Affordable option | More expensive |

Treatment for Hip Dysplasia in dogs
Vets usually prescribe non-steroidal anti-inflammatory drugs (NSAIDs) for minimal side effects. As all dogs are unique, you may find alternative pain medication to help regulate your dog’s condition.
Vet-approved joint supplements offer a boost for vulnerable joints, muscles, and connective tissues.
Omega-3 fatty acids, glucosamine, and chondroitin sulfate are often prescribed. Regular injections to replace joint fluid can be beneficial for excruciating symptoms.
Further scientific studies are exploring new ways of treating CHD. Recent theories propose platelet-rich plasma injections can relieve pain by supplementing joint fluid.
Hyaluronic acid (used in joint fluid) with stem cells has also been promising.
These treatments, in combination with regular physical therapy, keep your dog’s joints healthy. Professional physiotherapy, such as hydrotherapy, is particularly successful for dysplastic dogs.
A proper diet is the most cost-effective way to manage your dog’s orthopedic symptoms. It will also prevent the condition from becoming severe.
By maintaining your dog’s lean figure, you’ll prevent the accumulation of extra weight. Thus avoiding further damage to their brittle joints, bones, and ligaments.
Your dog’s diet should be rich in nutrition, so their bodies can maintain an optimal level of health.
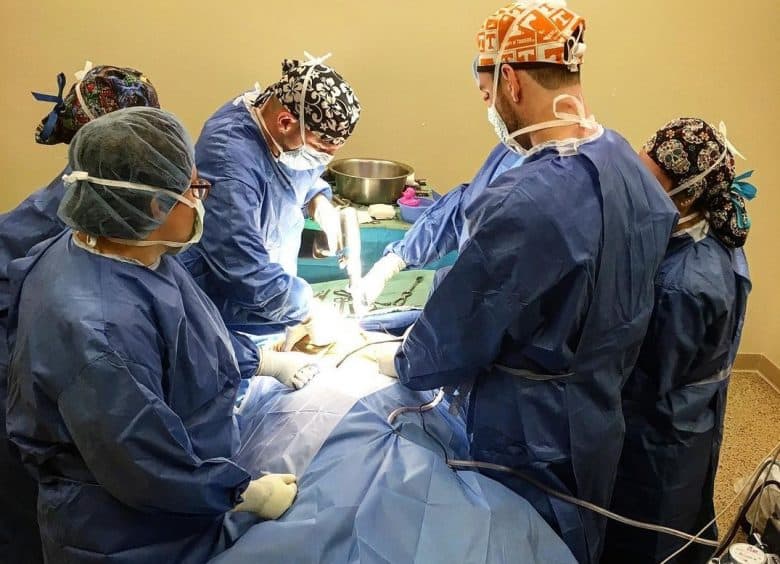
Surgical procedures for Canine Hip Dysplasia
For more severe CHD cases, surgery may be the best treatment option. There are several surgical procedures to choose from.
Your vet will determine what’s best for your pet depending on his or her pain levels, age, and lifestyle.
A diagnosis for CHD doesn’t always need surgery. As mentioned earlier, there are non-surgical routes to manage your dog’s symptoms.
But it’s good to know about last-chance treatment options if you do find yourself faced with them in the future.
Surgeries for Hip Dysplasia cost you between $1,500 to $4,500. Prices will be based on the type of surgery and your specific vet. The following are the common and successful surgical treatments for CHD:
- Juvenile Pubic Symphysiodesis (JPS)
- Total Hip Replacement (THR)
- Femoral Head Ostectomy (FHO)
- Double / Triple Pelvic Osteotomy (DPO/TPO)
As it happens, many fellow dog owners have found themselves wondering, what else can I do to ease my dog‘s pain?
Supplements, injections, and surgeries aside, there are alternatives to boost your dog’s health and manage their daily pain.
For example, mobility braces shift your dog’s weight to their front limbs. This helps relieve the joints from pressure.
Laser therapy helps manage inflammatory pain. It works by opening blood vessels and stimulating the lymphatic system.
It doesn’t have any reported side effects. Regular massages of the affected area can ease discomfort by stimulating blood flow.
Many pet owners have turned to Chinese medicine and acupuncture. These have helped to reduce inflammatory pain, increasing their dogs’ quality of life.
The best treatment for Canine Hip Dysplasia is often medical management.
Medical management means combining veterinarian-prescribed medicines, joint supplements, and health-promoting therapies mentioned above.

How can you reduce the risk of Hip Dysplasia?
Medication and treatment can’t prevent or fix all cases of CHD. Consistent management of your dog’s health can stop the disorder from becoming severe.
Specially-formulated puppy food for large breeds prevents excessive growth and weight gain. This food helps the joints to develop and prevent long-term problems.
The right amount of exercise promotes physical health and prevents obesity, but keep in mind that overexertion can damage puppies’ growing bones and joints.
Staying informed about Hip Dysplasia is helpful as an owner of an at-risk dog. NEVER skip your dog’s annual trip to the vet.
If he’s showing symptoms of having CHD, observe and take note of every single detail that happened or is happening. This will be useful during check-ups and treatment.
This is also why we can’t emphasize enough on buying puppies from responsible breeders who do genetic testing to ensure that their dogs are screened for hereditary diseases.
Life for dogs with Hip Dysplasia
This condition can be debilitating if left unnoticed and untreated. Many diagnosed doggies live long and happy lives.
Based on your dog’s clinical signs, you can identify a proper health plan, as well as manage your dog’s symptoms with help from your vet.
The CHD gene is polygenic, meaning the condition shows itself in many different ways. Symptoms will vary between individuals.
Some dogs appear pain-free for many years, while others can become affected early in puppyhood.

The verdict about Hip Dysplasia in dogs
As responsible owners, we want to ensure we identify any early signs of CHD. Know the difference between Juvenile and Mature forms of CHD, and remember that diagnosis requires specialized testing.
Regular visits to the vet can also help to see signs of this developmental disease.
If you really want a breed that’s prone to orthopedic issues, then hip dysplasia is always a possibility. Proper diet and moderate exercise are essential, as well as regular physical exams.
Several pain-management strategies and surgical procedures are also available to help dogs with CHD live a virtually pain-free life.
There is no set experience when it comes to CHD. We’d love to hear your tips and success stories about how you manage the effects of this disease. Leave a comment below and share your thoughts.
Further reading: Other diseases and conditions in dogs
Reference
- https://phys.org/news/2008-08-extent-inbreeding-pedigree-dogs-revealed.html
- https://www.ofa.org/recommended-tests
- https://antechimagingservices.com/antechweb/pennhip
- https://pets.webmd.com/dogs/guide/dog-pain-medications#1
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7070503/
Cess is the Head of Content Writing at K9 Web and a passionate dog care expert with over 5 years of experience in the Pet Industry. With a background in animal science, dog training, and behavior consulting, her hands-on experience and extensive knowledge make her a trusted source for dog owners.
When not writing or leading the K9 Web content team, Cess can be found volunteering at local shelters and participating in dog-related events.
